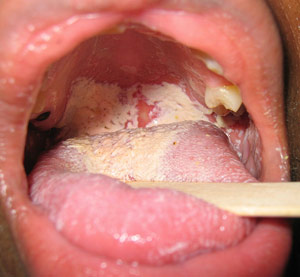
For the paper review, I chose the Gomaa et al. paper about the effect of hypertrophied (enlarged) adenoids on the voice and the mucosa of the larynx area in children.
The article can be found at http://dx.doi.org/10.1016/j.ijporl.2013.08.039
Introduction:
In this study, Gomaa et al. look at the effects of hypertrophied adenoids in children, specifically the effects on voice and the laryngeal mucosa. As discussed in my previous blog, the adenoids (or pharyngeal tonsils) are located in the roof of the nasopharynx. When adenoids become infected, a 'drip' of the fluid can land on the mucosa of the vocal folds causing irritation (leading to coughing). Hypertrophied adenoids are common in children and cause symptoms such as snoring, nasal congestion, obstructive sleep apnea and recurrent ear infections. Dysphonia, defined an audible change in a person's voice (either detected by them or someone else), is a common occurrence in children ages 8 to 14. Dysphonia in children arises from voice abuse and misuse from chronic upper respiratory tract problems, such as hypertrophied adenoids, which can cause an impact on the voice-related quality of life.
Methods:
Patients were chosen from the Department of Otorhinolaryngology at the Faculty of Medicine, Minia University from Nov. 2011 to May 2012. Two groups of children were used- 40 children who suffered from adenoid hypertrophy without any other causes of upper respiratory disorders (the patient group) and 20 children in the control group who did not have any upper respiratory diseases or hypertrophied adenoids.
Both groups of children had approximately the same mean age (6 to 7 years old) and the ratio of boys to girls used was about equal (slightly more girls in both groups). All subjects underwent a soft tissue X-rays as well as full history taking about history of dysphonia throughout life and family history of dysphonia or hearing loss.
To assess patients, a laryngeal telescope and a test called the auditory perceptual assessment (APA) of voice was done using a modified GRBAS scale. The scale for dysphonia and voice quality used were the grade of dysphonia, strained voice, leaky voice, breathiness and irregularness. To evaluate the APA, researchers looked at the grade of dysphonia, character of the voice (if its strained, heavy, etc.), pitch and loudness.
Data collected was analyzed using SPSS version 17, with Chi square tests being performed between many proportions and a p-value of <0.05 was used for significance.
Results:
Dysphonia:
Of the patient group, 6 had slight symptoms, 8 had moderate symptoms and the others did not show symptoms (35% of the patient group). The control group had only one child with slight symptoms. A p-value of 0.034 was determined showing an association between adenoid hypertrophy and dysphonia.
Leaky Voice:
Twelve patients suffered from leaky voice (30%) while none of the control did, so a significant association was made between adenoid hypertrophy and leaky voice was apparent (p=0.024)
Pitch of Voice:
Decreased voice pitch was also associated with adenoid hypertrophy with a (p= 0.011) as 35% of the patient group suffered from this while only 5% of the control group did.
Laryngeal lesions:
Laryngeal lesions were found on 32.5% of the patient group and only 5% of the control group, so a statistical association was made between adenoid hypertrophy and laryngeal lesions
Strained voice, breathiness, irregularity in voice and the loudness of the voice did not show significance for an association with adenoid hypertrophy.
Table 2 from the publication showing the significance in the results obtained
Discussion:
The author discussed current research complementing the research performed in this study. Multiple studies show relationships between nasal problems/obstructions and dysphonia. However the results from this study disagree with a previous study by Simoes et al. which showed breathiness in deviant voices but not vocal strain in voices. In this study, neither a strained or breathy voices were found to be significant amongst patients with adenoid hypertrophy, so further research should be conducted to determine if there is significance.
The author also mentions that endoscopy is the gold standard for research such as this, but due to the cooperativeness of children for semi-invasive procedures, is harder to perform procedures like these.
A main point discussed is that hypertrophy of the adenoids can lead to a higher tension in the laryngeal muscle and increase the sub-glottal pressure during speech, which may be a reason for the occurrence of leaky voice, congestion in vocal folds, thickening of the mucosa and nodules in the vocal folds. This agrees with the results found in this study as dysphonia, leaky voice and laryngeal lesions were found to be significant in children with adenoid hypertrophy.
Another idea arises from turbulence in airflow from the enlargement of the adenoid causing a lower pressure which in turn causes the voice to be altered leading to dysphonia and a more nasal-sounding voice.
Overall the research performed showed the importance of assessment of voice and laryngeal examination in children with adenoid hypertrophy. It was also determined that laryngeal lesions should be treated once the adenoids are removed.
Personal Critique of Paper:
When reading this article, one of the first things I noticed was the small sample size. Sixty children were used in total with 40 in the patient group and 20 in the control group. While this isn't an overly small sample, to draw significance and to be applicable to other research this experiment should be repeated with more subjects.
There wasn't much histological discussion about the laryngeal mucosa or adenoid hypertrophy in this paper. In general, there doesn't appear to be much histological information and pictures about the adenoid in the literature I used. When discussing the damage to the laryngeal mucosa, this paper would have better exemplified that by showing a comparison between damaged and non damaged regions.
There was three tables presented in the paper, with only one of them showing results obtained. I think this paper could have been better explained with some more graphs and figures.
Another problem I encountered while reading the paper was the modified GRBAS scale used as I feel not enough clarification was given on what counted as slightly, moderate, severe, etc. The scale may also be subjective as these categories could be interpreted differently by different experimenters. I also felt that not enough information was given about the characteristics of voice. It is hard to determine what counts as leaky voice is for example as no background is given for the four characteristics of voice. Overall, I found that the terms were not well defined, leading me to to more research about the topic.
I also thought there should have been more information on laryngeal lesions as they mentioned how there was a statistical association between them and adenoid hypertrophy. They mentioned minimal lesions are caused by adenoid hypertrophy and the importance of treating them, but this doesn't give the reader a clear idea on the reasoning of their importance. Also, the wording appears to be incorrect as on one page the author talks about how 32.5% of patients have laryngeal lesions and only 5% of the control does, while at the end, they say that laryngeal lesions only happen with adenoid hypertrophy, which doesn't support the previous statement.
Overall, I felt this paper needed some more clarification on how the scales were determined to test the subjects as well as clearer wording as I felt there was confusion with some main points.

.jpg)